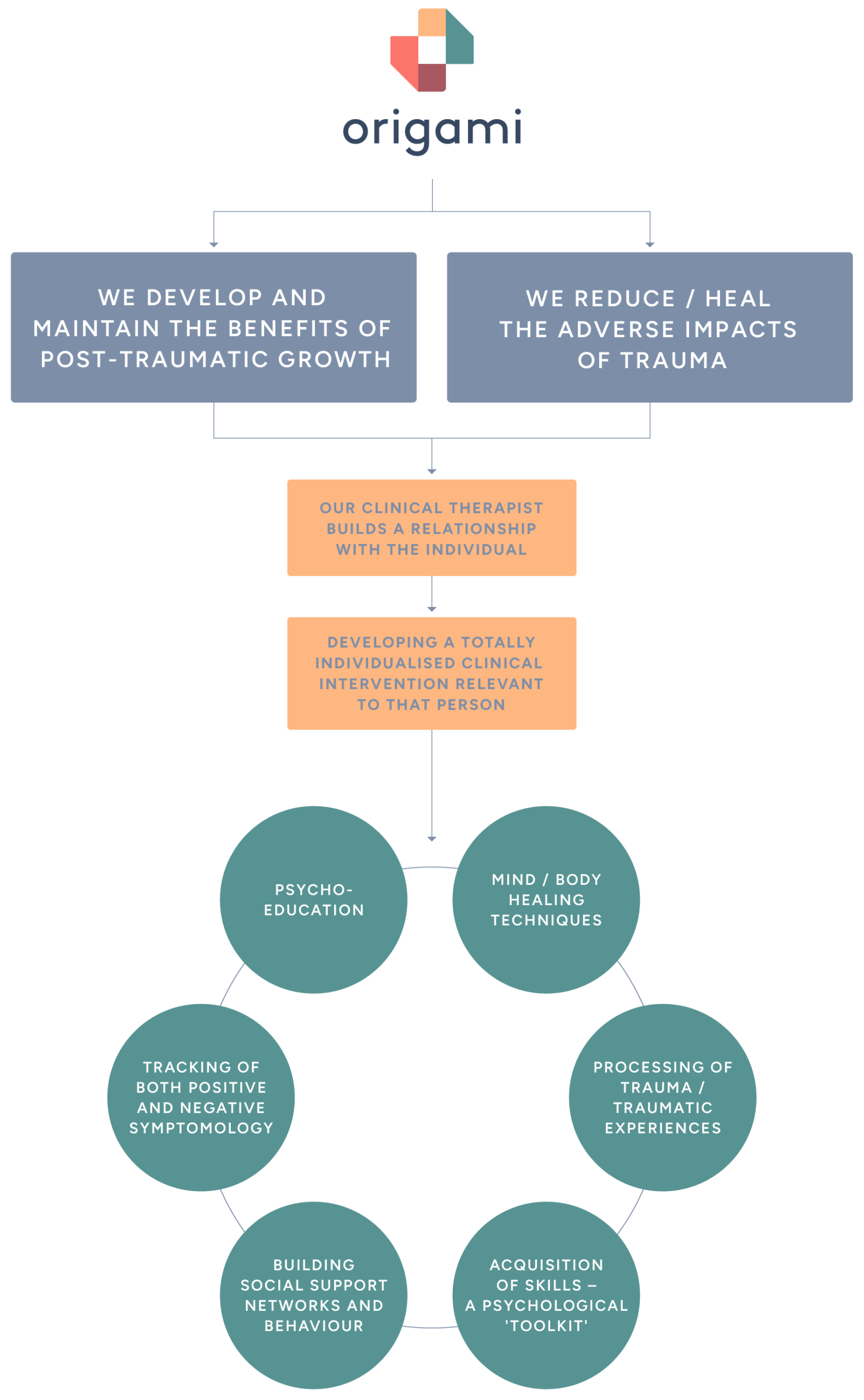
The neurobiological impact of trauma. It’s often assumed that post-traumatic growth (PTG) is purely beneficial, but research shows there can also be adverse or “costly” responses. Growth doesn’t always mean the nervous system has healed; sometimes resilience and lingering stress responses coexist.
Our developmental environment shapes neurological wiring. Neurobiological patterns, those organised sequences within brain and nervous systems, are critical for cognition, behaviour, and vulnerability to conditions. Early relationships mould the nervous system, and adverse childhood experiences are often sublimated in adulthood through coping strategies that enable adaptation and success.
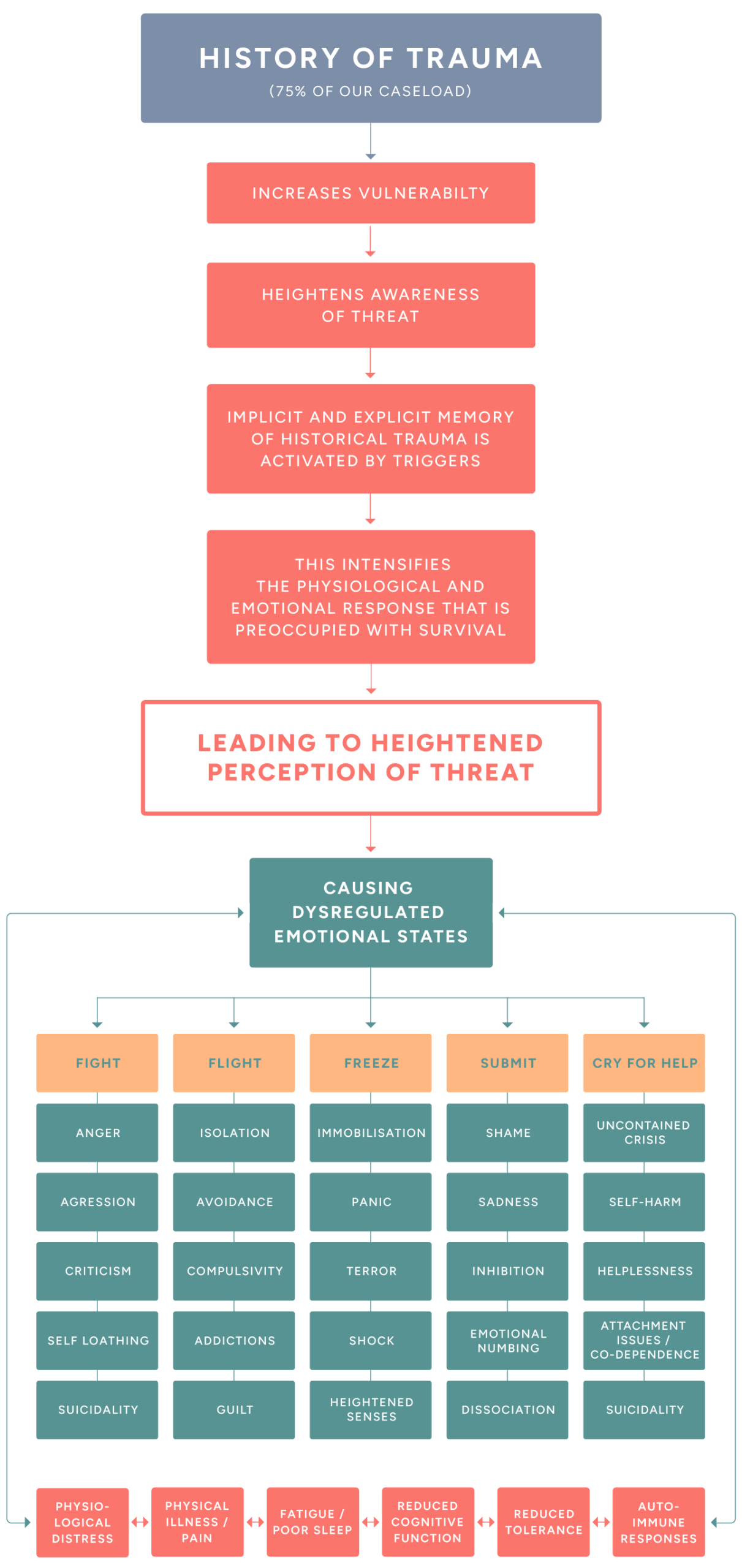
Yet these adaptive strategies can be triggered by adverse cues. While often useful, they may cross a fine line into problematic behaviours, straining both self and relationships. High functionality is sometimes correlated with rapid escalation of mental illness.
The main adverse correlates of PTG include:
- Physiological vulnerability despite psychological strength.
- Fatigue or executive function strain.
- Nervous system “primed” for threat, wearing down immunity and cardiovascular health.
- Over-striving, compulsive meaning-seeking, or “toxic growth.”
- Later vulnerabilities: anxiety, immune dysregulation, metabolic risk.
This coordinated stress response manifests as: loss of confidence, anxiety, hypervigilance, mistrust, overwhelming self-scrutiny, narcissism, boundary-poor relationships, lack of empathy, obsessive behaviours, sleep disruption, and severe physical or mental health issues.
In summary: Adverse neurobiological responses to PTG suggest growth may coexist with, or even depend on, residual stress signatures. Individuals may feel stronger and more purposeful, yet beneath the surface nervous, endocrine, and immune systems remain partly dysregulated, leading to exhaustion, absenteeism, early retirement, or even suicidality.